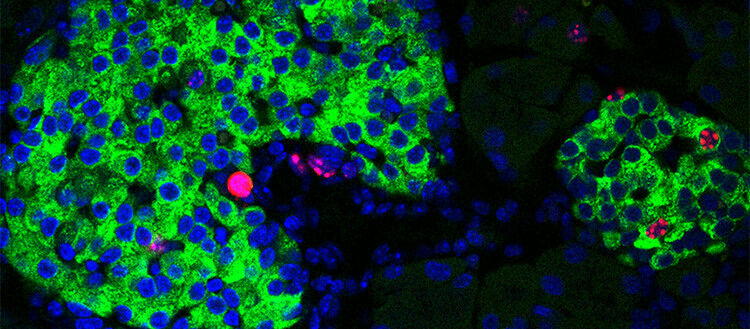
 Image of pancreatic islets with insulin-producing beta cells (green).
Image of pancreatic islets with insulin-producing beta cells (green).
By analysing the lipid profiles of dozens of people, UNIGE and HUG scientists have highlighted the importance of fat in the detection and treatment of type 2 diabetes. Image of pancreatic islets with insulin-producing beta cells ( green ). UNIGE / Dibner While sugar is the most frequently named culprit in the development of type 2 diabetes, a better understanding of the role of fats is also essential. By analysing the blood profiles of dozens of people suffering from diabetes or pre-diabetes, or who have had their pancreas partially removed, researchers at the University of Geneva and Geneva University Hospitals (HUG) have made two major discoveries. Firstly, the lipid composition of blood and adipose tissues fluctuates during the day, and is altered in a day-time dependent manner in diabetics, who have higher levels of toxic lipids. In addition, one type of lipid, lysoPI, is capable of boosting insulin secretion when the beta cells that normally produce it fail. These results, published in the journals Cell Reports Medicine and Diabetes , may have important implications for the treatment of diabetic patients.
PER LEGGERE QUESTO ARTICOLO, CREA IL TUO ACCOUNT
Ed estendere la vostra lettura, gratuitamente e senza alcun impegno.
I vostri vantaggi
- Accesso a tutti i contenuti
- Ricevere newsmail per le novità e le offerte di lavoro
- Pubblicare annunci


